Supporting Airway Management Providers in Emergencies
Evidence-based training for providers caring for critically ill patients in need of emergency airway management.

AIME for Airway Management Success
For more than twenty five years, Airway Interventions and Management in Emergencies (AIME) programs have supported clinicians worldwide augmenting their skills and confidence to manage critically ill patients in need of emergency airway management.
Created for physicians and other advanced providers working in acute care settings, AIME delivers practical, hands-on learning that reflects real-world challenges. Guided by expert educators who combine clinical excellence with engaging teaching, you’ll gain strategies that apply whether you work in a busy urban hospital or a remote community setting.
AIME Clinical Cadaver
-
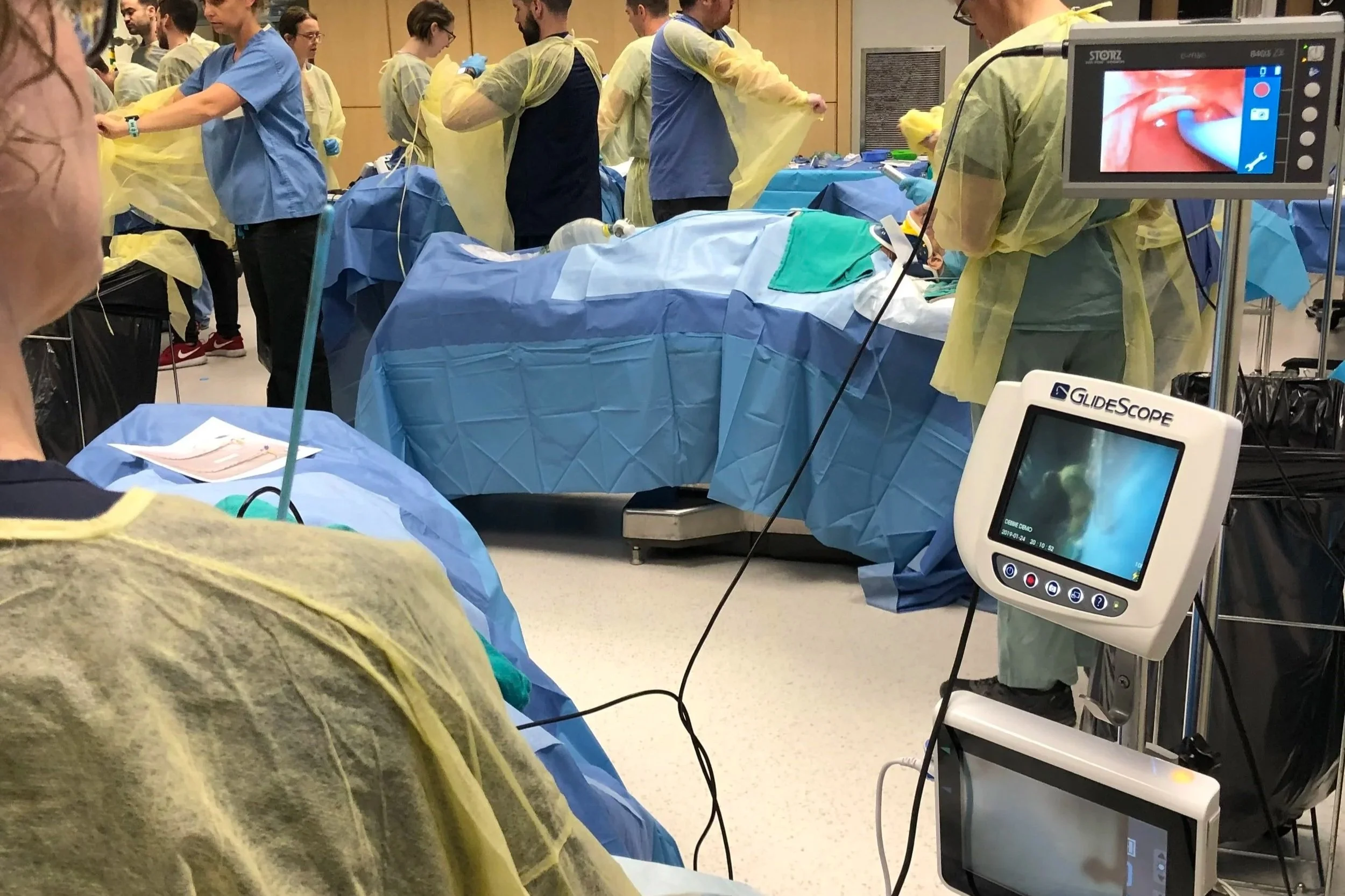
A Hands-on, Advanced Airway Learning Experience Using Clinical Cadavers
A procedure focused program offering unique repetitive practice opportunities that reinforce core and advanced airway skills using a variety of currently available and increasingly accessible airway devices. Attendees will learn not only from experienced airway educators that understand the varied practice environments clinician’s face but also from the greatest teachers of all, specially prepared clinical cadavers producing unparalleled high fidelity skills learning opprtunities.
AIME Awake
-
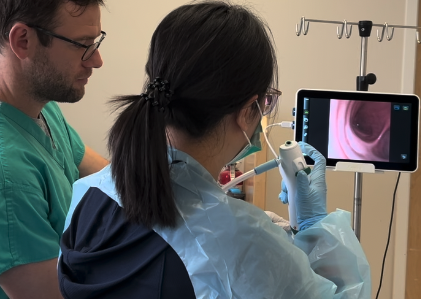
Making awake tracheal intubation a real option for managing the anticipated difficult airway in patient’s requiring emergency airway management
Guidelines for airway management in patients with an anticipated difficult airway universally include the option of performing an ‘awake’ tracheal intubation (ATI). Performing a rapid sequence intubation (RSI) using video laryngoscopy has become a standard approach to facilitate tracheal intubation for airway management in emergencies, whereas experience in performing ATI is limited. Awake tracheal intubation however remains a necessary alternative to RSI in not only anticipated anatomically difficult airway cases, but also for selected physiologically compromised apnea intolerant patients. This program provides attendees with with an approach and the skills necessary to safely perform ATI when indicated. Instructors from Emergency Medicine and Anesthesiology along with specially prepared clinical cadavers provide an unparalleled unique high fidelity skills learning experience.
AIME On-the-Road
-
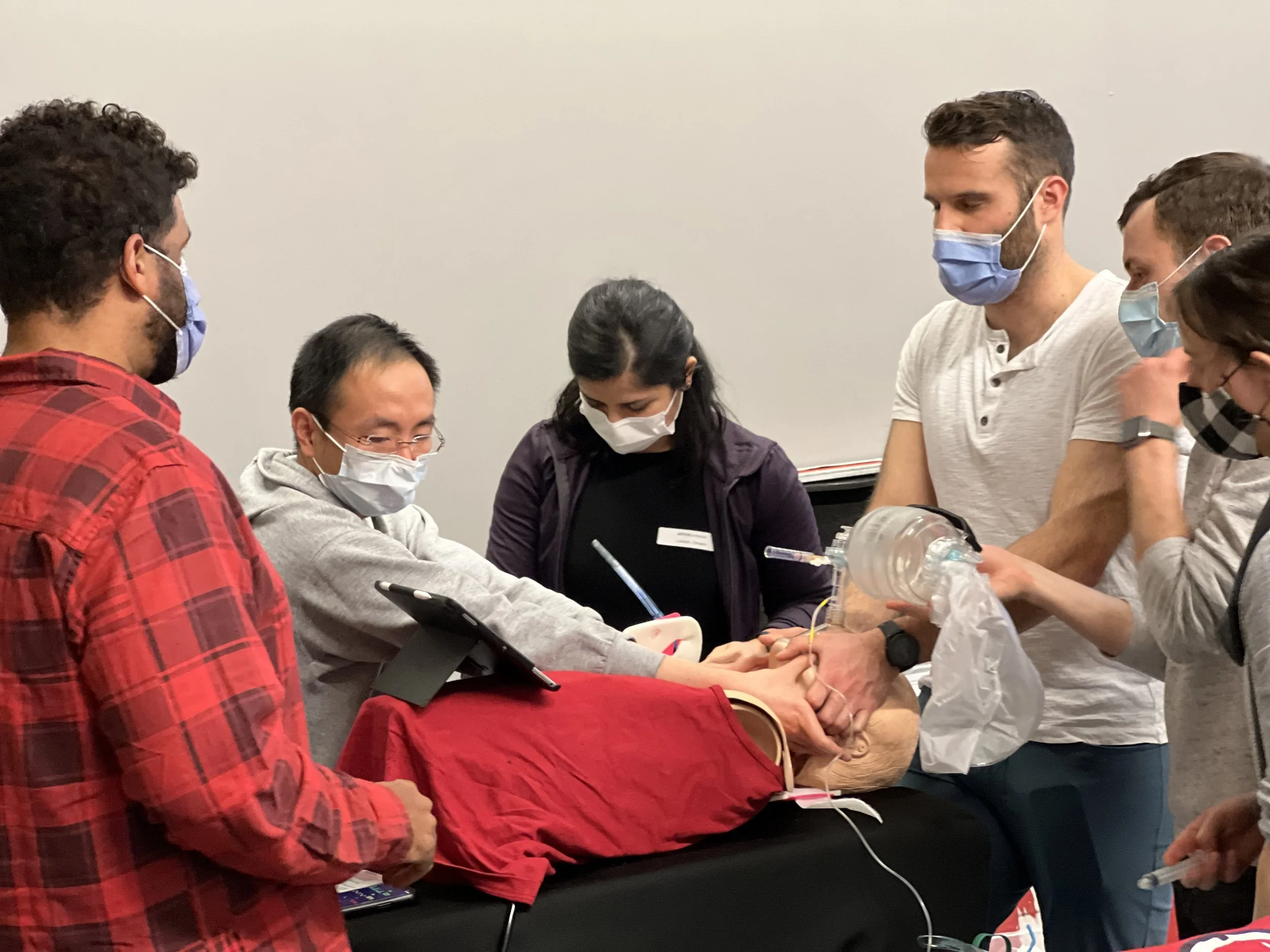
A Hands-on, Case-Based Practical Airway Learning Experience
For over 25 years AIME On-the-Road has been providing high value educational support for clinicians in Canada and other regions around the world who are responsible for airway management in emergencies. Management of both the anticipated and unanticpated difficult airway requires evidence-based decision making and skillful procedural execution customized the patient’s presentation and the providers clinical environment. This program uses case-based group discussion with hands-on workshops using commonly available/increasingly accessible airway devices with the goal of enhancing provider confidence and skills that ultimately improve patient outcomes.
